
CT Guided Liver Biopsy⁚ An Overview
A CT guided liver biopsy is a minimally invasive procedure where a radiologist obtains a small tissue sample using a needle. This process is guided by a CT scan, ensuring accurate placement and is crucial for diagnosing liver conditions, such as hepatitis or malignancy. The CT scan provides detailed images to guide the needle.
What is a CT Guided Liver Biopsy?
A CT-guided liver biopsy is a medical procedure where a small tissue sample is taken from the liver for examination. This technique employs computed tomography (CT) scans to provide real-time images, allowing a radiologist to accurately guide a biopsy needle to the targeted area within the liver. The process is minimally invasive, involving a thin needle inserted through the skin, which reduces the need for more extensive surgical procedures. The procedure is crucial for diagnosing various liver conditions, including infections, inflammation, and cancerous growths. By utilizing CT guidance, radiologists can precisely target specific areas of concern, ensuring the tissue sample is representative of the underlying issue. This enhances diagnostic accuracy, which in turn helps in planning the most effective treatment strategies. A CT guided liver biopsy is typically performed after consultation with a radiologist and is often used to assess both focal and non-focal liver lesions.
Purpose of CT Guided Liver Biopsy
The primary purpose of a CT-guided liver biopsy is to obtain a tissue sample for accurate diagnosis and assessment of liver conditions. This procedure is essential for identifying the underlying causes of liver abnormalities, such as hepatitis, inflammation, or malignancy. By using CT imaging, the radiologist can precisely target specific areas within the liver, ensuring a representative sample is collected. This is crucial for differentiating between benign and malignant conditions, staging the severity of liver disease, and evaluating the response to treatment. Furthermore, the biopsy can help in determining the extent and nature of liver damage, including fibrosis or cirrhosis. The results obtained from the biopsy are vital for guiding treatment decisions and establishing a comprehensive management plan. A CT guided liver biopsy is also used to monitor the progression of liver diseases, providing valuable information for making timely interventions and improving patient outcomes. The procedure plays a critical role in the diagnostic evaluation of both focal and diffuse liver lesions.
Procedure Details
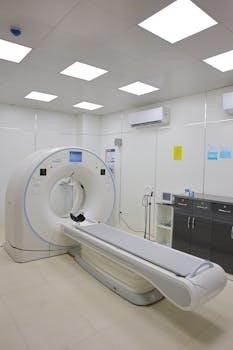
This section outlines the specifics of a CT guided liver biopsy, detailing how CT scans are used to guide the procedure, the sequential steps involved, and the specialized tools used. This will provide a clear understanding of the technical process used during the biopsy.
How is CT Guidance Used?
Computed Tomography (CT) guidance plays a pivotal role in liver biopsies by providing real-time, cross-sectional images of the liver. These images allow radiologists to precisely visualize the targeted area, whether it is a focal lesion or a specific region of the liver parenchyma. The CT scan helps navigate the biopsy needle through the abdomen, avoiding vital structures, such as major blood vessels and other organs. This accurate visualization minimizes the risk of complications and ensures the needle reaches the desired location with precision. The radiologist uses the CT images to plan the needle’s trajectory, adjusting it as necessary during the procedure.

CT guidance ensures that the tissue sample taken is representative of the area of concern, aiding in accurate diagnosis and the planning of appropriate treatment. Compared to blind biopsies, CT guidance significantly enhances the safety and effectiveness of the procedure. This imaging technique allows for the precise placement of the needle, which is paramount for obtaining a diagnostic sample and reducing potential complications. Utilizing CT scans, radiologists can monitor needle placement and the procedure in real-time, further increasing the effectiveness of the biopsy.
Steps in a CT Guided Liver Biopsy Procedure
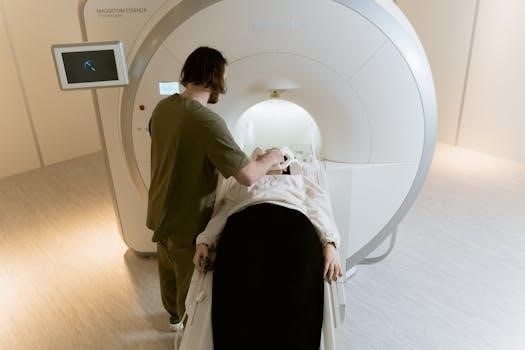
The CT-guided liver biopsy begins with a preliminary CT scan to locate the target area within the liver. The patient is positioned on the CT scanner table, and the area of the biopsy is prepped with antiseptic solution. Local anesthesia is administered to numb the skin and tissue along the needle’s path. Using the CT images, the radiologist plans the optimal needle trajectory, avoiding blood vessels and other vital structures. A small incision may be made at the entry site.
Under continuous CT guidance, the biopsy needle is advanced towards the target area. The radiologist monitors the needle’s position on the CT images and makes necessary adjustments. Once the needle is in place, a small tissue sample is obtained. The needle is then carefully removed, and pressure is applied to the puncture site to prevent bleeding. A dressing is placed over the area. The tissue sample is sent to the lab for analysis. The procedure usually takes a short time, often less than an hour, and patients can typically go home the same day, following a short period of observation.
Tools Used in the Procedure
The primary tool employed in a CT-guided liver biopsy is the biopsy needle, typically a fine-gauge needle, often 16G, designed to extract small tissue samples. This needle is specifically crafted for percutaneous procedures, meaning it’s inserted through the skin. The CT scanner itself is crucial, providing real-time images that guide the radiologist during the procedure. These images allow for precise needle placement, minimizing the risk of damage to surrounding structures.
In addition to the needle and CT scanner, other essential tools include antiseptic solutions for skin preparation, local anesthetic agents to numb the biopsy site, and sterile drapes to maintain a clean environment. Gauze and bandages are necessary for post-procedure care, applying pressure to the site and protecting it. Sometimes, a small incision is made using a scalpel to facilitate needle insertion. A contrast medium may be used in some cases to enhance visibility of the target area. Finally, the obtained samples are placed in appropriate containers for transportation to the pathology lab for detailed analysis, using specialized equipment.
Coding and Billing
Coding for a CT-guided liver biopsy involves two primary CPT codes. CPT code 47000 is for the biopsy of the liver, needle. CPT code 77012 is for the CT guidance during the needle biopsy. These codes are billed together.
CPT Code 47000⁚ Biopsy of Liver, Needle
CPT code 47000 specifically designates the procedure of a liver biopsy performed using a needle. This code is applicable when a percutaneous approach is utilized to obtain a tissue sample from the liver. This procedure is crucial for diagnosing various liver abnormalities, including inflammation, hepatitis, and malignancy. It involves inserting a needle directly into the liver through the skin. The sample is then sent to a pathologist for detailed analysis. This code represents the technical aspect of the biopsy itself, irrespective of the imaging guidance used. This code is often used in conjunction with imaging guidance codes, such as 77012 when CT guidance is involved. The use of a 16G core biopsy needle is often recommended for this procedure by many medical organizations. Code 47000 does not include the guidance component, therefore, it must be paired with another code to indicate use of a guiding modality. In essence, CPT 47000 captures the physical act of obtaining the liver tissue through a needle.
CPT Code 77012⁚ CT Guidance for Needle Biopsy
CPT code 77012 is used to report the radiological guidance for a needle biopsy procedure, specifically when computed tomography (CT) is used for imaging guidance. This code signifies that a CT scan was used to visualize the area of interest, and guide the biopsy needle to the correct location within the liver. This imaging technique enhances the precision of the procedure, reducing risks and improving diagnostic accuracy. Code 77012 is used in conjunction with the primary procedure code for the biopsy itself, such as 47000 for a liver biopsy. The radiologist uses the CT images to monitor the needle’s position in real time, ensuring it reaches the target tissue effectively. This code is crucial for billing purposes, as it reflects the specific service of providing the CT guidance during the biopsy. It is an essential component in coding a CT guided liver biopsy and should be reported separately from the actual biopsy procedure. This code ensures that the professional component of the radiological guidance is properly captured.
Considerations
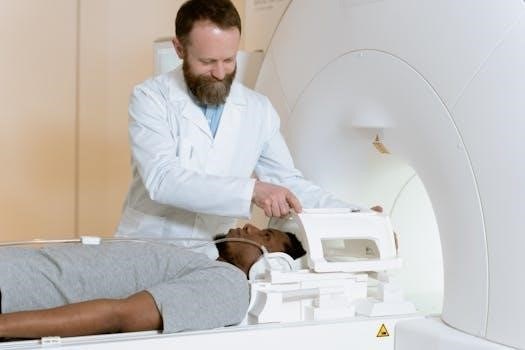
CT-guided liver biopsies may be combined with other imaging, like ultrasound. Risks include bleeding and infection. Benefits involve accurate diagnosis. These considerations help to assess the appropriateness of a CT-guided biopsy versus other methods and are essential for patient safety.
Combination with Other Imaging Modalities
While CT guidance is a common method for liver biopsies, it’s not always the sole imaging modality employed. In some instances, a combination of imaging techniques is used to optimize the procedure and ensure accurate tissue sampling. For example, ultrasound may be utilized initially to locate the lesion, followed by a CT scan to provide more precise guidance during the biopsy. This tandem approach can be particularly useful when dealing with lesions that are difficult to visualize using one modality alone. The initial ultrasound can offer real-time visualization, and then CT provides detailed cross-sectional images for exact needle placement. Additionally, MRI may be used to further characterize the liver lesions before a biopsy is performed, giving the radiologist more information to guide the intervention. The integration of different imaging techniques allows for a more comprehensive assessment, increasing the chances of obtaining a representative sample and minimizing complications. The choice of imaging modality depends on factors such as lesion size, location, and the patient’s specific conditions, making it crucial to tailor the approach for each individual case. This multi-modal approach is often used in complex cases to ensure the safest and most effective biopsy procedure.
Risks and Benefits of CT Guided Biopsy
CT-guided liver biopsy offers several benefits, including its minimally invasive nature, which reduces the need for open surgery. The precise guidance provided by CT scans allows for targeted tissue sampling, increasing diagnostic accuracy and minimizing the risk of missing the lesion. This is particularly crucial for small lesions or those located deep within the liver. The procedure is generally quick, taking only a few minutes for the actual biopsy, with minimal discomfort for the patient after the local anesthetic is administered. However, there are also some risks involved. These can include bleeding, which is usually minor but can sometimes be significant, particularly in patients with clotting disorders. There is also a small risk of infection, and damage to surrounding organs or structures, although this is rare when performed by experienced radiologists. Patients may experience some pain or discomfort at the biopsy site, but this is usually manageable with pain medication. The benefits of obtaining a tissue diagnosis often outweigh the risks and this is why it is generally considered a safe and effective procedure when performed by a skilled interventional radiologist. A thorough discussion of the risks and benefits with the patient before the procedure is essential for informed consent.